Cancer Cure Probable In 20 Years
Every single scientific discovery, big or small, can have a positive impact in the world. New technologies have been underpinning the western medical science. One such technology is promising a cure, almost, for the most-dreaded of human diseases – cancer.
The idea that a patient’s own immune system has the potential to attack and kill their cancer cells has been thought of, for a few decades, but in practice, it’s becoming a reality only recently. There was news in June 2018 when a team of US researchers led by Dr Steve Rosenberg at the US National Cancer Institute, has apparently cured a woman’s advanced breast cancer, by treatment with her own immune cells.
We human beings, as well as other lower forms of animals, have always been protected from diseases by our immune system generatedby the hundreds of million years of evolution. No creature big or small has been ignored. Augustus De Morgan wrote in 1872: “Great fleas have little fleas upon their backs to bite ‘em. And little fleas have lesser fleas, and so ad infinitum.”
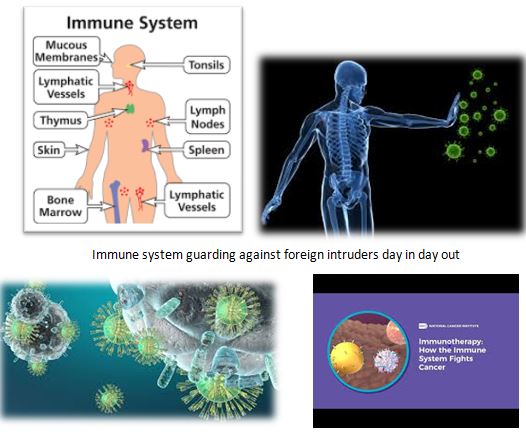
Our immune system guards our body 24 hours a day from ‘foreign intrusion’ into our body. It has the ability to adapt to strange changing environments. That’s why it’s critical in fighting infections and cancer. There’re different immune responses for different infections, and cancers. Our body cells have a marvellous capacity for renewal. If you are cut by a knife, your body will heal the wound by rapidly dividing themselves. Every time a cell divides, there is a small chance that it may develop an unpredictable alteration called ‘mutation’ that will transform it into a cancer. As an infection reproduces much faster than its hosts, an effective immune system is necessary to cope with it, unlike our heart or kidney that do the same job day in day out.
Our immune system is always on the prowl looking for “foreign intruders” or foreign bodies ie anything that is not part of the body, such as germs and other outside materials eg a life-saving organ transplant. It attacks to throw them out of your body (rejection). That’s why patients with organ transplants eg kidney, have to take drugs known as immune-suppressive drugs that block their immune defences all their life. This makes them vulnerable to infection. However, doctors are good in keeping a balance in giving you just enough medications to prevent organ rejection and make you less susceptible to infections.
In 1967, Dr Christiaan Bernard made the first heart transplant in South Africa. The operation was successful but the patient Louis Washkansky (53) died of pneumonia 18 days later. Since then thousands of lives have been saved with heart transplant with the right amount of immune-suppressive drugs. The Kidney was the first organ to be successfully transplanted in 1954.
Scientists are now using our immune system to tackle the challenge of rapidly evolving cancers, such as lung cancers. On December 27 2018, British scientists at the Francis Crick Institute in north London, announced a long-awaited cancer breakthrough.
Prof Adrian Hayday, an immunological expert, who leads the team, said doctors could become more like engineers, upgrading the body rather than bombarding it with toxic chemotherapy. He believes that it’s possible to strengthen the body’s defences by transplanting immune cells from strangers [that won’t be rejected by the patient].”
Chemotherapy kills rapidly dividing cancer cells. It also kills normally dividing and growing cells in the body, especially blood cells (causing anaemia) and intestinal cells (causing diarrhoea and vomiting) as well as hair root cells (causing baldness).
“Even a few years ago the notion that any clinician would look at a patient and deliver a therapy which wasn’t going to directly affect the cancer in any way, shape or form, would have been pretty radical. But that’s what is happening. We are seeing impressive results with cells called natural killer cells. It’s very early days but there are patients receiving them in this next year and the year after, and the nice feature is, unlike other immune therapy, these cells are not rejected [thrown out of the body],”
“So you have the possibility of developing cell banks that could be used for any one. You would call them up and deliver them to the clinic, just hours before they were needed to be infused. We aren’t quite there yet. But that’s what we are trying now. Until this year, scientists thought it would be impossible to import a stranger’s immune cells as the immunosuppressive drugs needed to ensure the body did not reject them, would cancel out the benefits. But in 2018, scientists realised that immune cells are unlike other cells, can survive well in another person, opening the door to transplants,” said Prof Hayday.
“In the UK, more than 350,000 people are diagnosed with cancer each year. Only one in four would have survived for 10 years, 30 years ago. But because advanced drugs, up to 50% survive today. We want to make that 75%,” added Prof Hayday.
I would like here, to explain what immune system is, what immune cells are and what they do in our body.
Immune system is the body’s defence against infectious organisms and other invaders eg a thorn, which our bodies regard as “foreign bodies’. It does a great service to human health and saves life. Without them evolution by natural selection would have gone an entirely different way. It’s partly because of its great adaptability to changing environments.
When a thorn is lodged in your body, our immune cells know it’s a foreign body and they immediately try to throw it out (reject) from its intrusion. So is a bacterial infection. They attack them ferociously. During the process, some immune cells sacrifice themselves, and along with the thorn or dead bacteria, bits of tissue and serum they form pus that surround the foreign body. With the pus they get ejected spontaneously or surgical incision, as in the case of an abscess.
When you have a routine blood test, doctors look for white blood cells (WBC) and red blood cells (RBC). RBC carry oxygen we inhale from our lungs. WBC protect us from foreign bodies. They are of five different groups. Out of these, immune cells known as Neutrophils and macrophages respond quickly to local attacks by intruders.
When infections that are not destroyed by these suicidal attacks, another group of WBC called lymphocytes will co-ordinate as they have functions of adaptation and memory. These ‘adaptive immunity’ cells known as T-cells and B-cells will make specific responses and will remember individual types of infections. For instance, a previous infection of typhoid fever will be membered and met with a faster and more effective counterattack.
Cells, the powerhouses in our body, work day and night to keep us going. These cells have hundreds of different types of ‘receptors’ on their walls. These are specialised proteins that allow communication of the inside of the cell with outside. They carry out fundamental functions like transporting glucose from our food into the cells. Those receptors associated with the immune system, are generally concerned looking for evidence of infection or abnormal cell death. When they find such a strange evidence, their job is to maximise the likelihood of the person’s survival by eliminating infection or cancer.
When it comes to cancer, the immune army doesn’t always win the battle and we die. Even a virulent infection can make such profound changes on our body that the imprint of individual pathogens can be observed in the tree of evolution. Analysis of inheritance has shown how co-evolution of host and infection has altered the make-up of our immune system and cell receptors in recognising and fighting disease-causing germs.
New immunotherapy treatments along with new technologies are now going to give the immune system better arsenal to do the job it was meant to ie fight back against threats like cancer. Our immune system is a complex apparatus that both protects the body and, in some cases, helps to destroy cancer.
Prof Charlie Swanton, of the Cancer Evolution Laboratory at Francis Crick Institute, finds the discovery very hopeful: “In recent years it has become clear that every tumour is made up of many different groups of cancer cells, each with their own unique genetic makeup but all related to each other. Some groups of tumour cells develop resistance to treatments such as chemotherapy, immunotherapy, radiotherapy and targeted therapy, meaning that when the cancer comes back it is harder to treat.”
Prof Swanton and his team will begin trial next year, to see if ramping up these specific cells could be effective in fighting lung cancer, by expanding these tumour cells from the patient’s tumour in the lab and giving them back to the patient in hopefully overwhelming numbers to tackle the tumour at its trunk. He said: “between 1980 and 2010, 519,000 cancer deaths were avoided because of cancer research. If that’s not for optimism I don’t know what is.”
He continued: “I would go as far as to say that we might reach a point, may be 20 years from now, where the vast majorities of cancers are rapidly treated diseases or long-term chronic issues that you can manage. And I think the immune system will be essential in doing that.”
Image Credit: pixabay.com
Website: drimsingh.com
